The Importance of Effective Patient Care Management in Healthcare

Practices with effective care management programs can address health risks and decrease costs. These strategies help to deliver on the Triple Aim of healthcare.
However, the execution of these efforts can take time and effort. Effective patient care management requires several components, including historical and real-time data, a robust risk stratification process, and effective tools for communication.
Patient-Centered Care
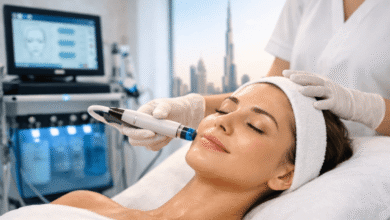
Patient-centered care is a collaborative model that builds meaningful relationships between patients and clinicians. It focuses on the patient’s patient’s needs and wants, and it addresses their social determinants of health to achieve better outcomes.
Both parties benefit when patients and clinicians work together: patient satisfaction increases, and healthcare providers gain more knowledge about the patient to tailor their treatment. It also reduces medical costs, as a study shows that doctors who communicate well with their patients use fewer diagnostic tests and hospitalizations but also receive more referrals from satisfied patients.
Patient-centered care focuses on building trusting relationships with patients by empathizing and establishing eye-to-eye communication during visits. It also involves sharing detailed, unbiased information about medications, physical limitations, dietary restrictions and more to empower them to make informed choices that align with their values and priorities.
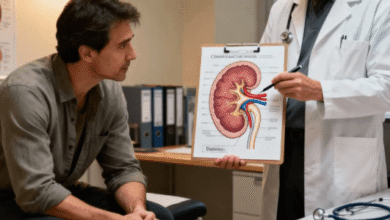
Coordinated Care
Poorly coordinated care can be safe and even deadly for patients. It can also increase costs and lead to unnecessary procedures. With proper patient care coordination, clinicians may get important information about a patient’s health history or a specific medication, or they might order duplicate tests or prescribe medications that could interact with other treatments.
In addition, patients might visit multiple specialists and healthcare systems and need clarification on how to make appointments or when to follow up. This can lead to patient confusion and frustration, disrupting clinician schedules and wasting time.
Effective practices develop a comprehensive patient care management plan that includes patient-centered goals and implement the plan sustainably when grant funding expires. These successful practices often engage patient advocates, usually licensed social workers, who communicate with patients and their families to ensure they understand their plans and expectations. They also provide referrals to support services.
Cultural Competence
Cultural competence describes the attitudes, behaviors, policies and structures that come together in a system, agency or among professionals that enable effective work cross-culturally. It refers to an integrated pattern of human behavior that includes thoughts, communications, actions, customs, beliefs and values of a racial, ethnic or religious group.
NPIN reports that some research shows that culturally competent health care improves patient outcomes and decreases disparities. Increasing cultural competency has several benefits, such as better communication between physicians and patients. Having a clear dialogue also helps prevent medical errors and safety concerns.
NPIN outlines five elements of cultural competence:
- Value diversity
- Self-assessment
- Managing the dynamics of difference
- Acquiring and institutionalizing knowledge about culture and cultural contexts
- Systematically involving consumers, families and communities
The organization also suggests that training focuses on priority populations beyond racial/ethnic minorities and persons with disabilities, such as LGBTQI. These groups are often overlooked in the literature, and only some culturally competent interventions are available.
Patient Engagement
Patient engagement requires active participation by patients and includes discussion, decision-making about treatment options, and participation in each care step. Health professionals define engagement at the individual level (related to treatment) and organizational (related to quality improvement).
It’s essential to recognize that not all patients are willing or capable of engaging with their healthcare. There are both personal and systemic barriers that prevent many individuals from being proactive. For example, not all individuals have the health literacy or digital access necessary to be engaged. Also, not all individuals are comfortable sharing their concerns with their physicians for various reasons like age, gender, religion, or culture. Fortunately, modern tools allow healthcare organizations to easily, conveniently, and securely provide patient engagement. These platforms enable individuals to book appointments online, view their medical records, update their personal information, and communicate with their physicians. As a result, engaged patients are less likely to cancel or miss appointments